Trigger finger surgery
During trigger finger surgery, an incision is made in the narrowed pulleys around the tendon sheath that bend the fingers, causing the complaints, after which the free movement of the tendons is possible again, restoring the full range of motion of the finger.
What is a trigger finger?
The trigger finger (digitus saltans) is one of the most common lesions on the tendons caused by tenosynovitis of the hand, accompanied by changes in the tendons running on the hand and a narrowing of the pulleys surrounding them.
It got its name after the characteristic snapping sound and sensaiton that can be observed when the fingers are stretched out.
Its development is most common in women between the ages of 40 and 60, but nowadays it also affects an increasingly younger age group due to the excessive use of electronic devices.
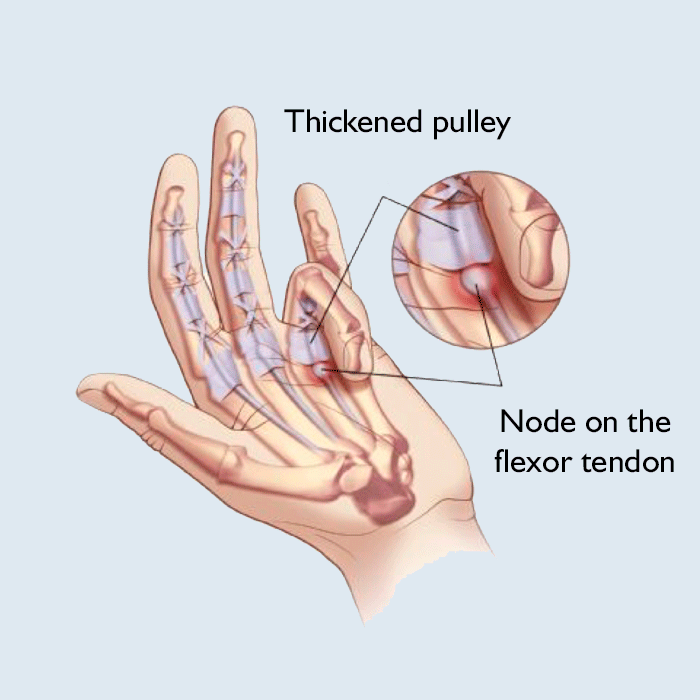
How does it develop?
The movement of our fingers is helped by ligaments that move the bones according to muscle function. Its flexors run through a passage, the tendon sheath, from the forearm muscles to the fingers. The inner surface of the tendon sheath is slippery, allowing the tendons to slip.
A trigger finger develops if a thickening or lump is formed on a short section of the tendon, or if inflammatory deposits or thickening occur on the inner surface of the pulleys.
When the finger is moved, this thickened tendon should slide through the narrowed section of the passage, causing a snapping, crackling sensation in the finger and a distinctive sound.
When tendon movement becomes difficult or gets stuck, it causes further inflammation and swelling, leading to an increase in complaints as a pathological cycle. Sometimes the finger gets stuck permanently, in which case it locks in a folded or extended position.
The reasons for its formation are not clear, it can be caused by overloading the hand, monotonous, constant movements, mild injury of the palm, which irritates the flexor tendons, scarring and also predisposing to certain diseases (diabetes, arthritis).
What are the symptoms of trigger finger?
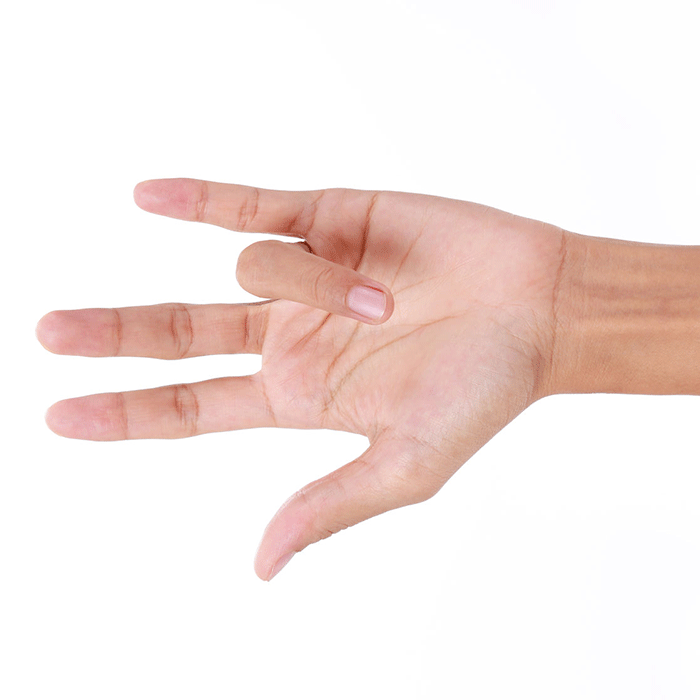
The first symptoms of trigger finger are pressure sensitivity at the base of the fingers, pain, and palpable swelling at the base of the fingers on the palm side caused by the thickened tendon sheath. The narrowing develops here, but the snap that occurs when the finger is stretched is felt in the middle phalanx in case of long fingers and in the distal phalanx of in case of the thumb.
The affected finger is more difficult to move when bent, the patient may feel it thickened.
The symptoms intensify in the morning and then, by moving the finger during the day, they alleviate but do not go away.
In the absence of treatment, the symptoms may increase, making it even more difficult to move the finger, and the patient may only be able to bend it from the extended or bent position with the other hand.
How to treat a trigger finger?
In all cases, the goal of the treatment is to dissolve the block of the flexor tendon and restore the range of motion of the fingers.
If you consult a specialist in the early stages of the disease, conservative (non-surgical) treatment can eliminate the complaints. The treatment aimed at eliminating the inflammation of the tendons is done by resting (using fixatives) and using locally applied anti-inflammatory creams and patches. If appropriate, treatment with steroid injection may be supported.
In addition to conservative methods, trigger finger treatment can also be performed surgically.
When is trigger finger surgery warranted?
Surgical treatment of the trigger finger becomes warranted if the disease interferes with the patient’s daily activities, conservative treatment has failed, or recurrent complaints are encountered, or if the finger has become completely immobile.
How is the surgery performed?
During the preoperative consultation, the hand surgeon will provide detailed information about the necessary preoperative tests, as well as the course of the surgery and its risks. Trigger finger surgery is performed under sterile surgical conditions, under local anaesthesia, as part of a day surgery.
During the operation, the hand surgeon makes a cross-section of 1-1.5 cm above the opening of the affected tendon sheath, and then splits the tendon sheath ring lengthwise, which eliminates the narrowing. The incision is made in case of the long fingers along the palm of the hand, parallel to it, and in case of the thumb, at its base. Any mucosal proliferation that may have developed around the tendon will be removed at the same time during surgery. Finally, the surgeon closes the wound.
After a few hours of observation after surgery, the patient can leave for home.
What are the dangers of surgery?
Like all medical interventions, trigegr finger surgery can have dangers and complications. Very rarely, inflammation and infection of the surgical site, as well as damage to the surrounding anatomical formulas: tendons, muscles, blood vessels, nerves, and adjacent bones, can occur. In such cases, medication may be required in milder cases and repeated surgery in more severe cases.
A more serious complication is purulent inflammation of the operated area, which can be avoided by fully adhering to hygienic rules.
What can I expect after the surgery?
The sterile, surgical dressing should be replaced the next day if the bandage is not damaged, in the uncomplicated case no further dressing is required until the suture is removed. The sutures are shown 8 to 10 after surgery. days are removed, hand sparing is recommended in the period before suture collection. Until the suture is removed, the wound should not be exposed to water, soaking of the dressing should be avoided. Regular exercise of a previously obstructed finger is recommended after the operation, the movements to be performed can be learned from a physiotherapist.

In some cases, senistivity, pain, and swelling may persist after surgery, to varying degrees. Complete recovery takes 3-6 weeks, and then daily hand use gradually becomes possible as the pain subsides.
