Dupuytren’s contracture surgery, fascia excision
During the Dupuytren’s contracture surgery, the contraction of the palmar fascia is released or removed, depending on the stage of the lesion.
What is Dupuytren’s contracture?
Dupuytren’s contracture, also known as the contraction of the palmar fascia, is a disease of the layer of tissue that lies beneath the skin of the palm of the hand. It causes abnormal thickening and contraction of the fibrous connective tissues of the palm, causing the fingers to bend inwards and often preventing them from functioning properly.
Rarely, the condition can affect other parts of the body: it can manifest itself in the form of lumps on the back of the finger joints (Garrod’s pads), lumps in the arch of the feet (Ledderhose disease), or beneath the skin of the penis.
What causes Dupuytren’s contracture?
The exact cause of Dupuytren’s contracture is unknown. However, some risk factors have been identified. Genetic predisposition seems to play a role in the development of the condition, as Dupuytren’s tends to run in some families. Northern European ancestry is also a risk factor, some hypothesise that the prevalence of the deformity in certain areas could be explained Viking migration.
Dupuytren’s contracture forms due to the benign tumour of the palmar fascia. The contracture first presents as a thickening or nodule in the palm, which is usually painless. After a while, these nodules form a thick cord which in later stages starts to gradually contract the finger(s) inwards towards the palm. In most cases finger the ring finger is affected, followed by the little finger, and sometimes the middle finger. Often both hands are affected, but the contracture is usually more advanced on the dominant hand.
It typically develops in men around the age of 30-40.
There is evidence that Dupuytren’s contracture is more likely to develop in people who have diabetes, smoke, drink, patients with epilepsy and those who have previously suffered trauma to the hand. The disease is progressive, without treatment it gets gradually worse until the patient is no longer able to use the affected fingers at all.
What are the symptoms of Dupuytren’s contracture?
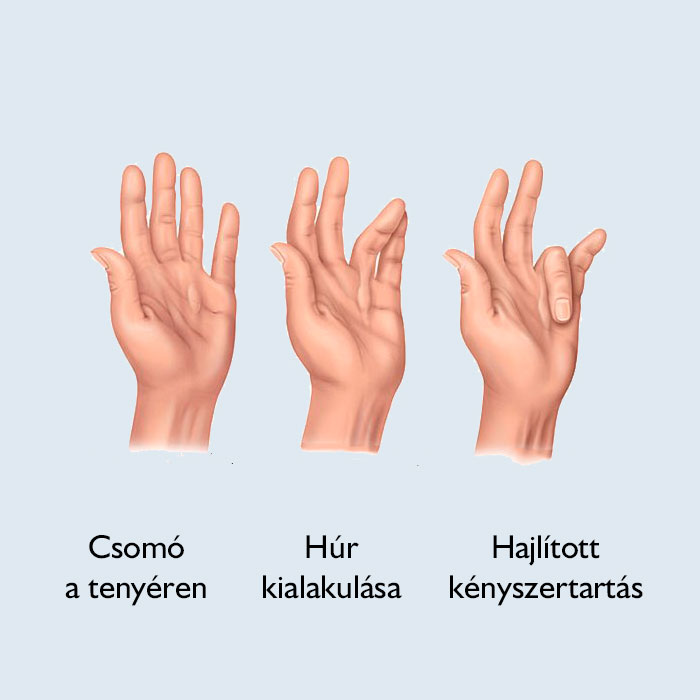
Dupuytren’s contracture has different symptoms at each stage. The condition usually begins as a thickening of the skin on the palm. As it progresses, the skin can appear puckered or dimpled. A firm lump of tissue may develop which may be sensitive to the touch but usually not painful.
At the next stage, cord-like lumps of tissue form under the skin of the palm which can extend up to the fingers. As these cords gradually tighten, the range of movement of the fingers becomes more and more limited. Most patients visit an orthopedic specialist at this stage. In more advanced stages of the disease, the fingers might be pulled inwards towards the palm. In some cases the fingers stop moving altogether.
Dupuytren’s contracture develops slowly, over several years, but it is difficult to predict how the condition will progress. Some people have only small lumps or cords while others go on to develop severely bent fingers.
How can Dupuytren’s contracture be diagnosed?
A physical examination is sufficient to diagnose Dupuytren’s contracture. An orthopaedic specialist or hand surgeon can diagnose the lesion after visual inspection and palpation, no other examination is usually needed to establish the diagnosis.
How can Dupuytren’s contracture be treated?
The treatment of Dupuytren’s contracture depends on the stage of the condition.
At an early stagae, if the hand function is good and the lumps are not causing any pain or inconvenience, observation is enough.
Steroid injections may help reduce the inflammation. If the cords are already formed, but the movement of the fingers is not significantly limited, physiotherapy can help slow the progression of the contracture fingers.
If you have difficulty using your fingers, fasciectomy is recommended.
When is surgery recommended?
Dupuytren’s contracture is a progressive disease. This means that the condition gets gradually worse and this process cannot be reversed by conservative treatment such as rest or medication. If the complaints have a significant impact on the patient’s ability to carry out their daily activities, the movement of the fingers is limited or the contracture is in an advanced stage and the fingers are completely bent towards the palm, surgical intervention is recommended.
What happens during surgery?
The surgery is performed under general, regional or local anesthesia depending on the severity of the contracture. During the intervention, blood flow to the hand is blocked temporarily in order to protect the surrounding nerves and blood vessels.
In milder cases, the surgery is performed under local anesthesia. The contracted fibrous tissue is cut with a needle or through a tiny incision.
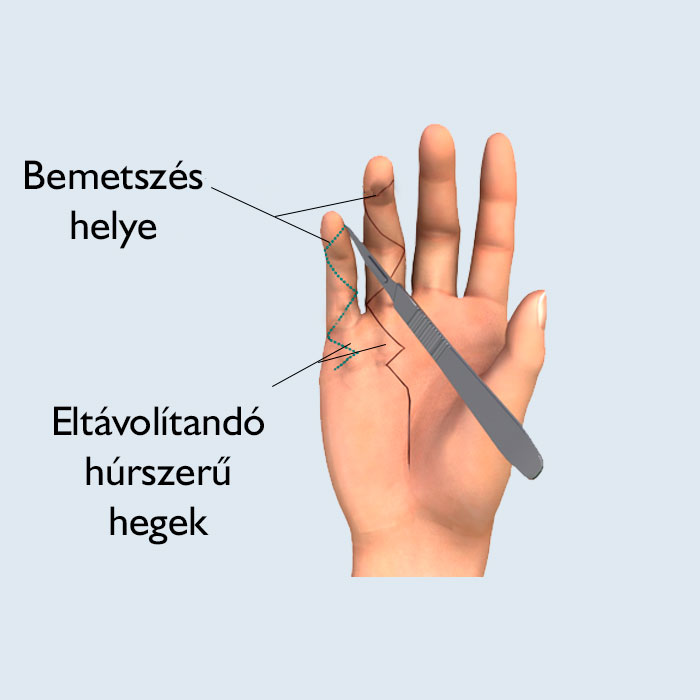
If the contracture is in an advanced stage, fasciectomy is performed while the patient is under general anesthesia. The surgeon makes Z-shaped incisions on top of the cord, removes the affected connective tissue, and releases the joint capsule. A skin graft is sometimes required to seal the wound.
What are the risks of the intervention?
As with any medical procedure, Dupuytren’s contracture surgery can have risks and complications. Very rarely, inflammation and infection of the surgical site and damage to the surrounding anatomical formulas (tendons, muscles, blood vessels, nerves) can occur. In such cases, medication may be required in milder cases and repeated surgery in more severe cases.
What to expect after surgery?
The surgical procedure is followed by a follow-up treatment, the effectiveness of which requires the active cooperation of the patient.
Dupuytren’s contracture repair is performed as one-day surgery. After a few hours of monitoring, you will be ready to leave the hospital. However, in case of a severe contracture, where the cords have been removed, 24 hour monitoring is recommended.
The bandage has to be changed on the next day, suture collection takes place 10 days after surgery. Until then, your hand should not come into contact with water.
After cord transcision, normal use of the operated hand can be resumed on the next day, while in case of cord removal, or major surgery, you have to wait for the wound to heal completely. After three to four weeks, the patient can start exercising their hands to achieve the best possible functional result.
In both cases, special hand and finger exercises are recommended for 3-4 weeks after surgery to facilitate recovery.

The wound may remain swollen, sensitive and painful for a few days after surgery.
Full recovery takes about 3-4 weeks after cord transcision, and 8-12 weeks after cord removal.

