Rheumatology
Rheumatology deals with the conservative, non-surgical treatment of the parts of the musculoskeletal system (tendons, muscles, ligaments) besides the joints, and spinal lesions.
Orthopaedics deals with the restorative and surgical treatment of acquired and congenital musculoskeletal disorders (implantation of prostheses, bone and cartilage replacement, corrections).
With what complaints should you see a rheumatologist?

- Joint pain (shoulder, wrist, ankle, knee, hip, elbow) that does not result from injury
- Pain, tenderness, swelling and redness suggestive of arthritis
- Cracking when moving joints
- Long-standing joint stiffness, which in addition to pain, already restricts movement
- Back and spinal pain
- Muscle pain
- If osteoporosis is suspected
Treatments available at our Clinics
Physiotherapy
Therapeutic massage
Within the framework of electrotherapy:
- Ultrasound treatment (both dry and underwater)
- Electrotherapy treatments (Iontophoresis, Interference, selective stimulus current, TENS, galvanic)
Immediate pain relief if needed
- Steroid and non-steroidal sedatives
Cure-like injection treatments
- Injections into joints, muscles and vertebral skeletal muscles
Cure-like infusion treatments for musculoskeletal problems
- Sciatica infusion
- Neodolpasse infusion
There is no extra charge for steroid injection, it is included in the price of the examination.
The course of the rheumatological examination
During the rheumatological examination, the specialist first asks the patient about the complaints (exactly where, how long and how often the pain occurs, whether a trauma affected the certain part of the body, whether an insect bite had happened before the complaint occurred, or whether there is an accompanying symptom), previous illnesses, medications taken, and family illnesses. This is followed by a general physical examination: the rheumatologist inspects the affected part of the body, checks its range of movement, muscle strength, reflexes, and locates the pain by palpation. Depending on the complaint, the rheumatologist checks the condition of the spine and gait, possible postural abnormalities and a neurological examination may also be performed.
The rheumatologist may request a laboratory or additional imaging (ultrasound, X-ray, MRI, CT) and bone density measurements to make the diagnosis, which are available at our Clinic.
What diseases does the rheumatologist treat?
Degenerative joint diseases are treated within the framework of a rheumatology clinic, if they do not require surgical intervention:
- spondylosis: involves the reduction of the distance between the vertebrae and calcification of the ligaments connecting them. The mobility of the spine is therefore significantly reduced. It can also affect the lower, middle and cervical sections of the spine.
- arthrosis: a degenerative joint disease in which the cartilage covering the surface of the bones in the joints becomes thinner. The joint may be painful, swollen, deformed, and its range of movement is narrowed.
Rheumatologists should also be consulted when it comes to painful conditions of the spine (e.g. lower back pain, pinched nerve, lumbago), and osteoporosis should also be diagnosed and treated within the framework of a rheumatology clinic.
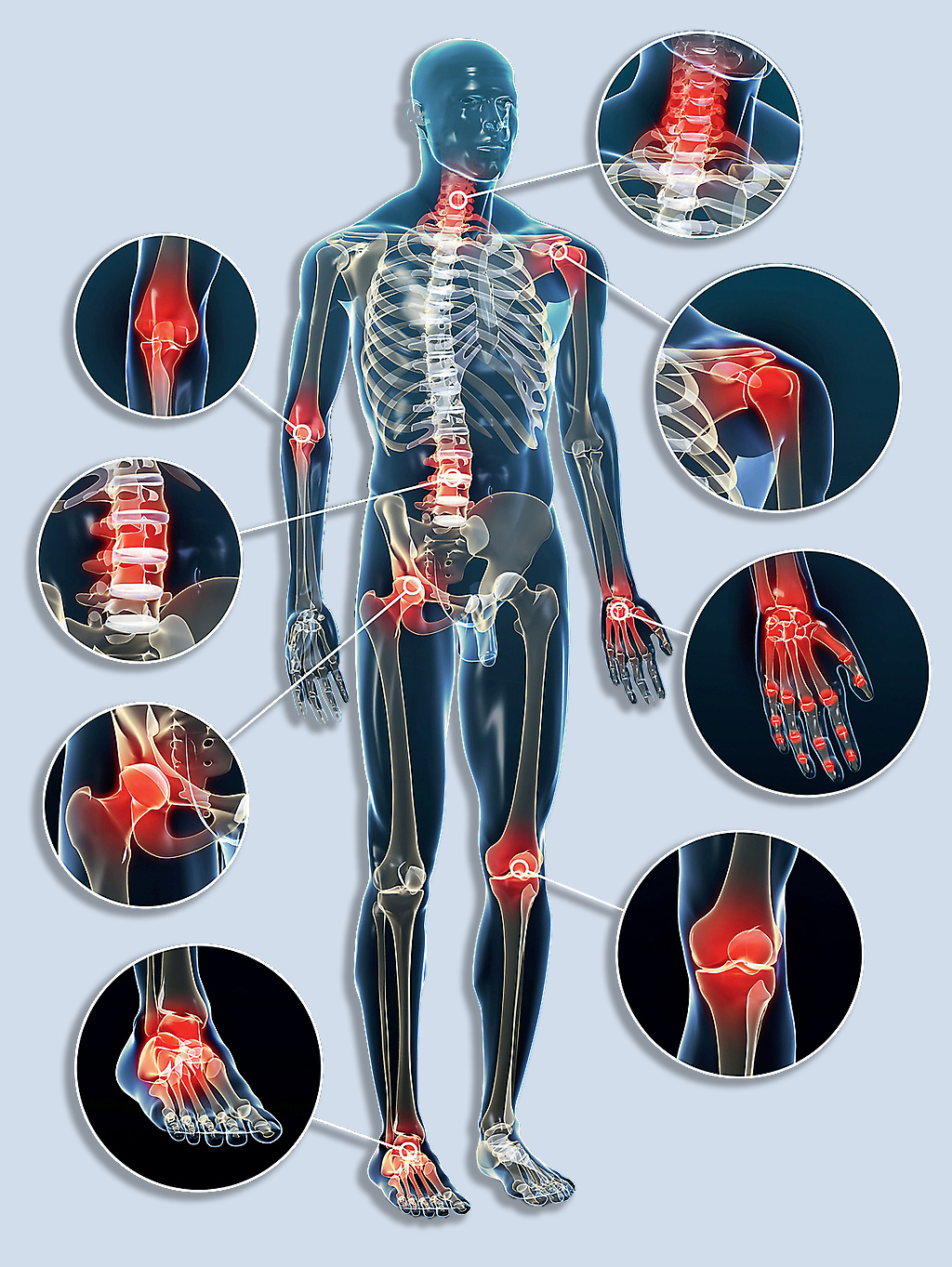
The rheumatologist deals with diseases that cause musculoskeletal complaints.
- rheumatoid arthritis: due to inflammation, accompanied by the thickening of the joint membrane, the joints become swollen and deformed.
- tendonitis: may occur on the hands, wrists, feet, and ankles due to overexertion. The tendon sheath swells, and the consistence of the substance helping the tendons move changes, which causes severe pain when moving the limb.
- gout: a disease caused by a metabolic disorder in which the presence of elevated uric acid results in the deposition of uric acid salts (sodium urate) in the joints, causing their inflammation.
- lupus (SLE): this autoimmune disease is associated with general symptoms (fever, diarrhoea, weakness), which is accompanied with symptoms associated with an organ attacked by the immune system. Most often, joint complaints (stiffness, pain, limited mobility) are characteristic.
- Bechterew’s disease: calcification of the joints between the vertebrae, and the sacral and hip bone, as a result of which the spine becomes completely stiff. Predisposition to the disease can be determined by laboratory testing of a blood sample.
- Sjögren’s syndrome: an autoimmune disease that causes painful polyarthritis among other symptoms, depending on whether the disease also affects gland function (if so, dry eyes and dry mouth, dry airways, dry skin can occur).
- halisteresis (osteomalacia): a disorder of bone metabolism. It is caused by a mineralization disorder that occurs during bone formation, as a result of which the mineral content of the bones changes, therefore the strength of the bones decreases significantly.

