Lumbar disc herniation (discus hernia lumbalis) surgery
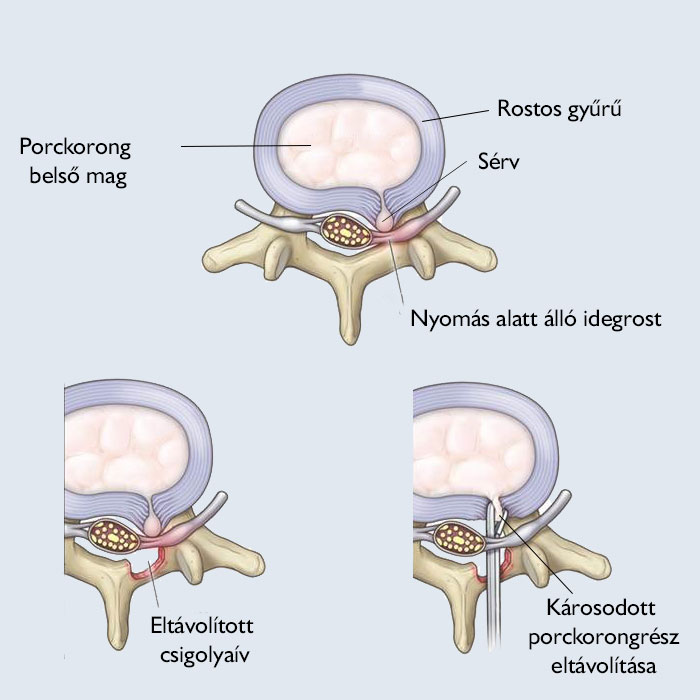
As we age, and due to increased physical exertion, the water content of intervertebral discs decreases, as well as their elasticity, their structure changes and they wear out. As a result, the fibrous wall of the disc may weaken, which might result in the protrusion of the disc wall. Additionally, the wall of the disc can rupture, and the elastic material inside the disc can break through the gap, resulting in a hernia. Protrusion or herniation of the disc can lead to a narrowing of the space (in the spinal canal or along the root canals leading to or from it) and to pressure on the nerve fibres, which can cause numbness, pain, loss of muscle strength, paralysis and, in more severe cases, paralysis and urinating and defecating difficulties, and impotence in men.
In the long run, damage to the disc results in the loss of the connection between the vertebrae, which can be accompanied by other lesions in addition to injury.
When is lumbar disc herniation surgery necessary?
Surgery is rarely needed in cases of disc herniation (approximately 2%). If the symptoms and complaints do not improve in 6-12 weeks, or even worsen during this time, therefore since the complaints do not improve with non-surgical, i.e. conservative treatments, we offer surgical solution. For pain that does not respond to conservative treatment, consideration should be given to surgical intervention.
In more severe cases, when there is a sudden symptom of more severe nervous system damage (more severe muscle loss, paralysis, urinary and defecation disorders, limb clumsiness, dysbasia), surgery is urgently needed within 24-48 hours because after this time frame, the chance of improvement reduces.
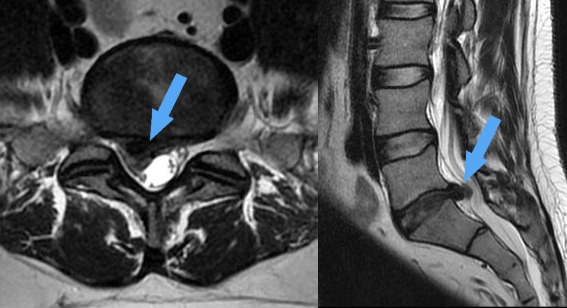
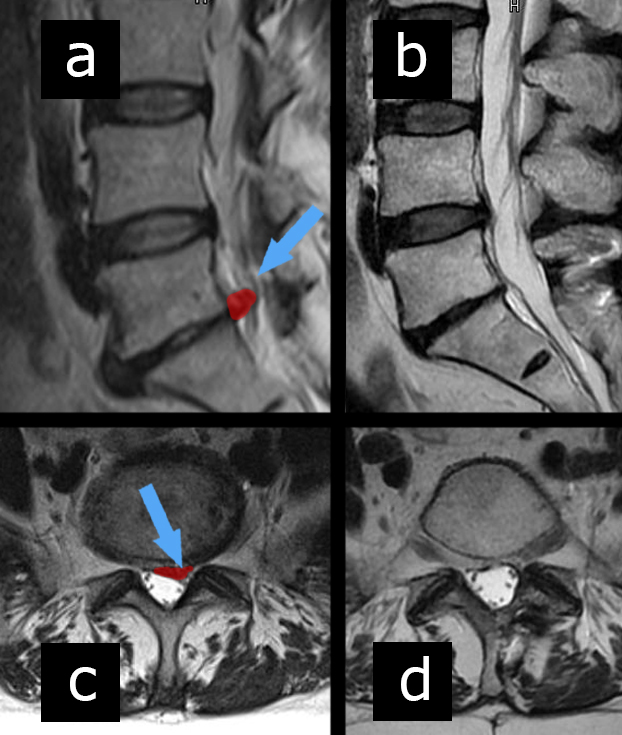
The MRI image (a) shows a side view of the lumbar spine. Arrow points to the disc herniation between the 5th lumbar vertebra (L5) and the 1st section of the sacrum (S1), and the disc herniation was painted in red. (c) is a cross-sectional MRI image also showing the hernia in red and a blue arrow pointing to the hernia. Figures (b) and (c) show the condition after hernia removal.
(Source: http://gerincsebeszbudapest.hu/ )
How is lumbar disc herniation surgery performed?
Removal of the disc herniation causing the pressure of the nerve element (nerve root, cauda fibre) from the posterior, open, mini-excision (approx. 3-6 cm), release of the nerve element under anaesthesia – called microdiscectomy.
In the case of a hernia in the spinal canal and the root canal accessible from the root canal, the procedure is as follows:
During lumbar disc herniation surgery, we reach the spinal canal through a small incision, by gashing the fascia that is located in the middle, posterior zygapophysis of the vertebrae, by detaching the muscles, with the removal of the ligamentum flavum connecting the vertebral arches, and by removing minimal parts of the bone of the vertebra above the vertebral arch and the inferior articular process.
We lift the strained nerve root from the hernia. From the spinal canal, we take out the embossed or torn disc(s), thus releasing the pressed, strained nerve root and radicals. Damaged disc parts are removed from the inside of the disc as needed. If necessary, the bone-constricted spinal or root canal is dilated by removing the constricting bone elements. In the surgical area, a suction tube (drain) is left behind, and we close the wound above the drain.
In case of a disc herniation at or beyond the outer end of the root canal, the procedure of lumbar disc herniation is the following:
An incision is made on the skin in the lateral direction from the midline, with about 2 transverse fingers, and the spine is also exposed by slitting the fascia and separating the muscle fibres lengthwise.
In this case, we look for the root canal and the disc herniation stretching under the vertebrae on the side of the hernia where the small joints connect the vertebrae. During the opening, we pass between the lateral protrusions of the vertebrae (processus transverus), drill a part of the joint protrusion and thus reveal the outer end of the root canal, if necessary from there the edge of the spinal canal.
The herniated disc is then removed, thereby releasing the compressed, strained nerve root. Damaged disc parts are removed from inside the disc. In the surgical area, a suction tube (drain) is left behind, and the wound is closed above the drain. The duration of surgery is 45-60 minutes, the hospital stay is 2 days.
What to do after lumbar disc herniation surgery?
Physiotherapy is required after surgery. If possible, do not expose the wound to water until the sutures have been removed. From the day of surgery until full mobility is achieved, injection therapy is needed to prevent blood clots (thrombosis). The recovery period is 6 weeks, but full recovery takes about half a year.
What are the advantages of lumbar disc herniation surgery?
Release of the neural formula (s) may reduce pain in the waist and lower limbs, reduce sensory disturbances or improve muscle strength, and normalize urinary and/or defecation disorders associated with the hernia. Surgery provides an opportunity to avoid possible subsequent paralysis.
What are the risks of the intervention?
In rare cases, there may be significant blood loss, cauda fiber damage (1-2% chance), decreased muscle strength, in more severe cases paralysis, sensory disturbances, joint sensory disturbances, incoordination. Postoperative haemorrhage of the surgical site, lower back pain, and recurrence of the hernia might occur.
Am I fit for lumbar disc herniation surgery?
In each case, your doctor will decide, based on preliminary tests, what the risk of your disc herniation surgery is. An anaesthesiologist is also consulted to determine the risk more accurately. The results of the tests and consultation with the anaesthesiologist are crucial.
What is included in the price of the lumbar disc herniation surgery at Medicover Hospital?
The cost of lumbar disc herniation surgery includes the cost of the surgery as well as the cost of the hospital stay after the surgery and the follow-up examination.
The implant to be implanted will be determined during the consultation by the specialist performing the surgery, depending on the case. The price indicated on the page does not include this fee.
The price of the preliminary specialist consultation and the pre-operative examinations is not part of the surgical fee, please inquire about the cost of these from our Call Center.
Convenience services
We accommodate our clients in a modern, pleasant, air-conditioned single room. Each room has a private bathroom, fridge and TV, as well as free WIFI access. We also provide our clients with individual nurse supervision, who will help your continuous recovery during your stay.

