What is colonoscopy?
Colonoscopy is an endoscopic examination of the colon (and the last section of the small intestine, i.e. the ileum). During the procedure, an endoscope, a flexible tube with its own light source, is inserted through the anus into the colon, at the end of which is a camera. The instrument is also suitable for tissue sampling (biopsy) and removal of polyps.
With the help of the camera, the intestinal mucosa can be examined in a well visible way in multi-magnification on a monitor, as well as minor interventions (biopsy, polyp removal) can be easily performed.
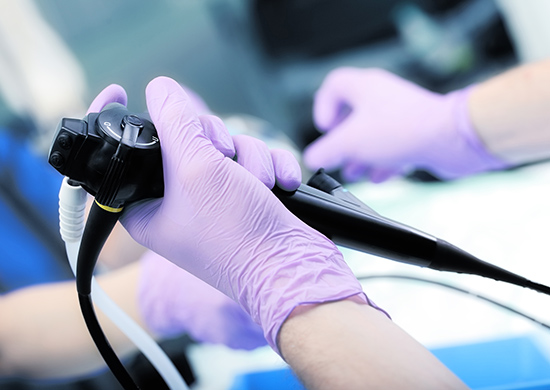
When do we perform colonoscopy?
Colonoscopy may be ordered by a specialist after the gastroenterological examination in case of the following complaints and symptoms:
- abdominal pain
- bloody stools or after positive bloody stool test
- persistent constipation
- diarrhoea
- change in bowel habit
- suspected inflammatory bowel disease (ulcerative colitis, Crohn’s disease)
- or as part of a colon cancer screening test
In addition to diagnostics, therapeutic intervention (polyp removal, haemostasis, biopsy for histological examination) may be performed during the examination.
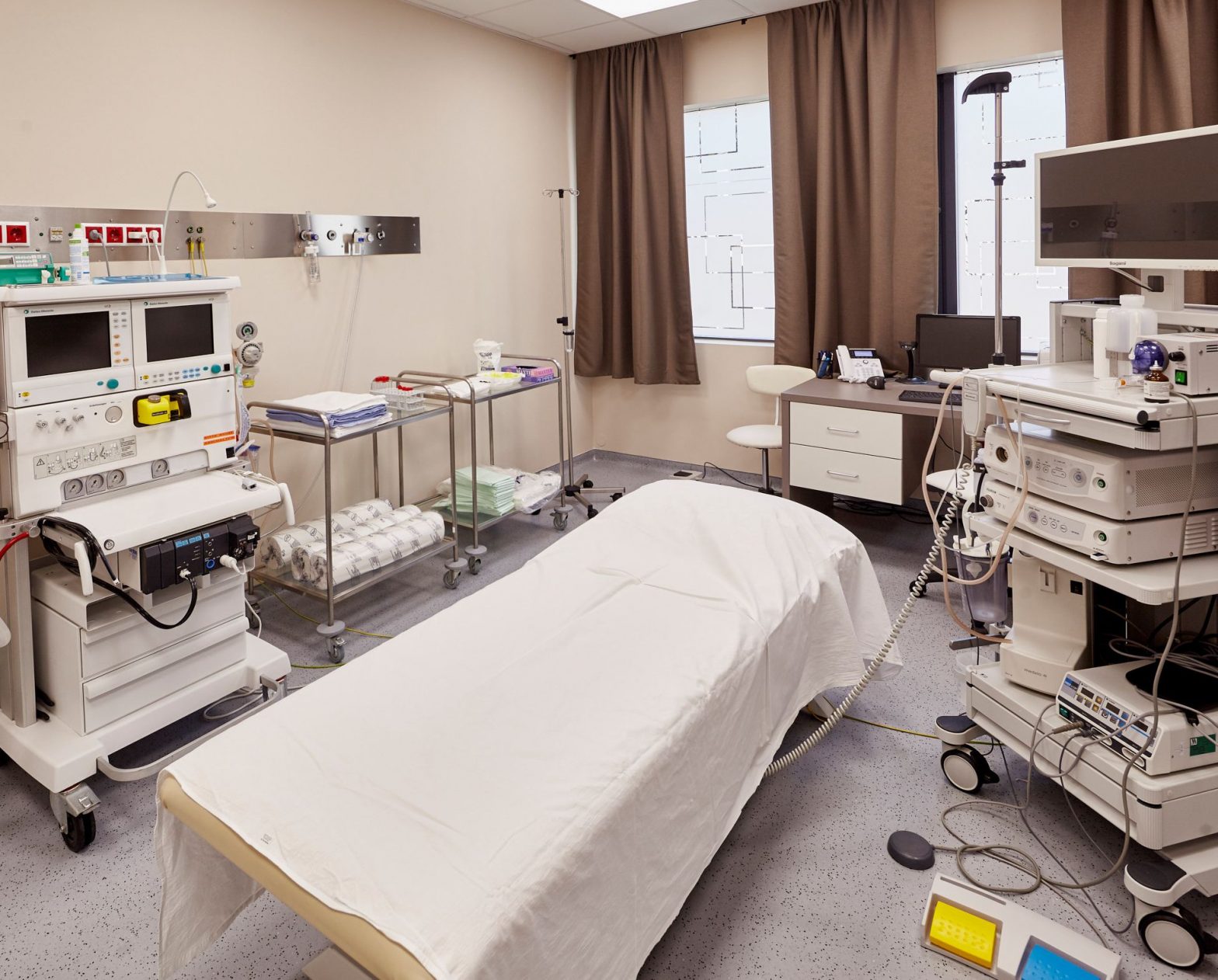
What is the process of gastroscopy?
During the examination, the patient lies on their left side with their legs pulled up. During the examination, the patient should turn to the back, possibly to the right side or, rarely, to the abdomen with the help of an assistant. The device is lubricated with a gel and then gently inserted into the rectum. During the examination, the anus is dilated by blowing air into it and occasionally by water.
During the examination, the patient may experience an urge to defecate provoked by the device, abdominal bloating and cramps due to the blown air, and abdominal pain because of the tension in the intestines. In patients where abdominal surgeries have caused intercrescence, these complaints are more common.
Pharmacological preparation may cause dizziness, nausea, vomiting, and hiccups.
After the examination, the patient will receive a finding immediately, if histological sampling has been performed, the result is expected in 1-2 weeks.
If a therapeutic intervention has taken place, institutional monitoring may be required depending on the risk factor.
During the examination, intestinal perforation and bleeding at the site of the polyp removal might occur as complication. The latter can usually be treated endoscopically, the former requires surgery.
Preparations
The examination requires 3-4 days of dietary (low-fibre diet) and pharmacological (laxative) preparation. Generally, we recommend consuming only soup at noon the day before the test and then taking a laxative. It can be any preparation of suitable strength, currently the most common are castor oil (which due to its oily texture can interfere with viewing and in many cases cause nausea and vomiting), flavoured, prescription solutions, and phosphor soda preparations. After that, it is recommended to drink large amount of fluid (water, tea) to completely cleanse the intestines.
Prior to therapeutic interventions, knowing blood counts, bleeding and coagulation parameters (blood sampling) and temporary discontinuation of anticoagulant (Syncumar, Marfarin), antiplatelet therapy (Aspirin, Astrix) are required.
After colonoscopy
Colonoscopy is usually performed under general anaesthesia with an anaesthetic-analgesic injection. After that, a short period of monitoring and rest is required.
Due to the use of anaesthetic injections, the patient is strictly allowed to leave only with an escort, and in this case, it is forbidden to drive.
Following colonoscopy, the patient can eat as usual at home, but an additional few hour of rest and consumption of plenty of fluids is recommended, and strenuous activities should be avoided. Unless you receive any other advice from your doctor, you can continue your usual daily activities 6-12 hours later.
Is colonoscopy dangerous?
Colonoscopy is a safe examination when a trained and experienced specialist and well-equipped and modern instruments are used.
Very rare complications may include colon damage or perforation of the its wall (which can occur when it has thinned due to a tumour or inflammatory disease in the intestinal wall).
In general, however, the diagnostic value of an endoscopic examination overshadows any inconveniences associated with the examination.

