Diagnostic hysteroscopy
When is it necessary?
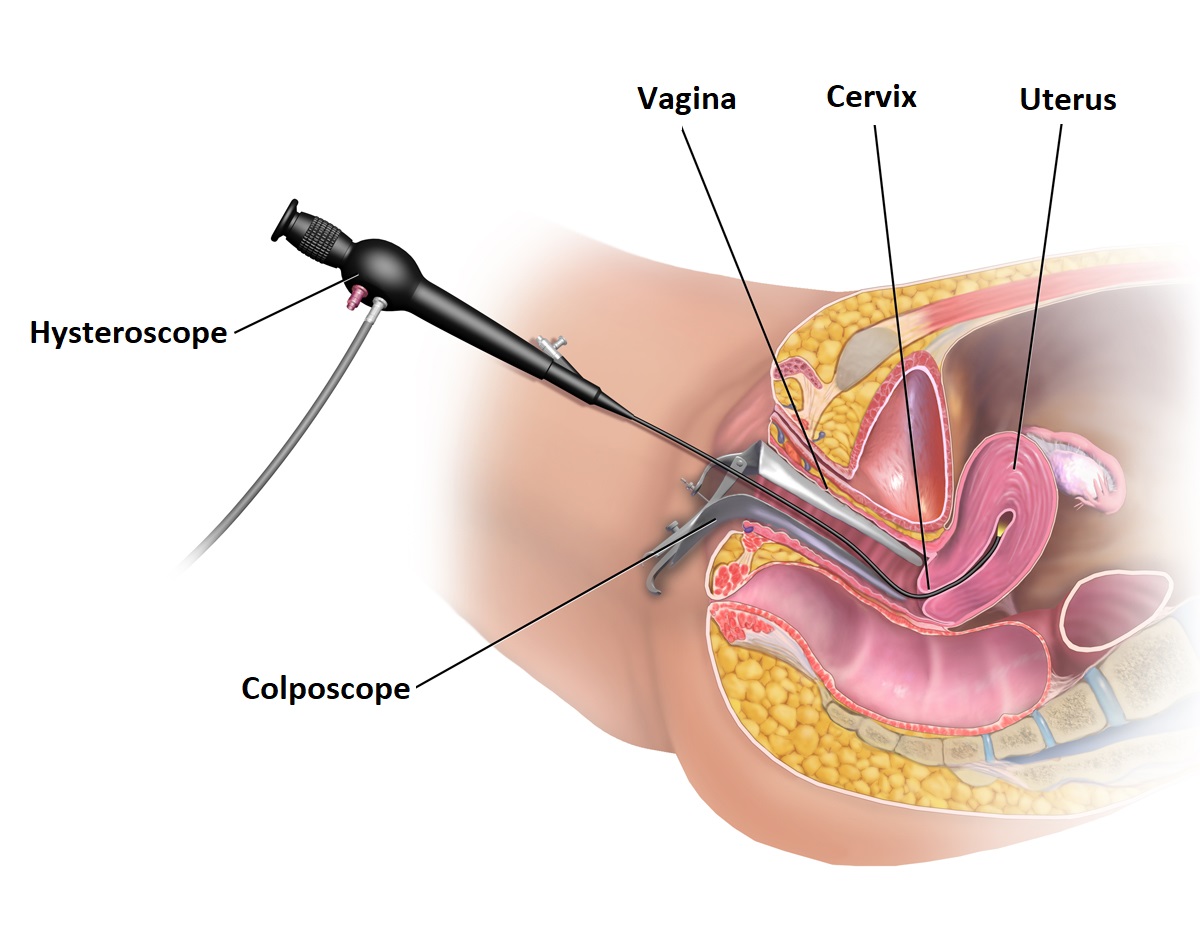
Hysteroscopy is an examination of the uterine cavity with a special endoscope (hysteroscope), which is inserted into the uterine cavity through the vagina, cervical os, and then the cervix.
In the case of diagnostic hysteroscopy, it is possible to examine the mucous membranes and tissues of the uterus thoroughly to rule out or confirm benign and malignant lesions.
Complaints indicating intervention
- other diagnostic examinations (ultrasound, X-ray, CT, MRI) suggest intrauterine lesions (myoma, polyps, tumours)
- in case of recurrent miscarriages to find out the causes
- bleeding disorders (especially after menopause)
- in case of infertility
- intrauterine foreign body (intrauterine contraceptive device, „spiral”)
How does the intervention go?
During the examination, it is possible to treat the detected lesions surgically (operative hysteroscopy).
Surgery can usually be performed under intravenous anaesthesia or local anaesthesia in combination with mild sedatives. After proper preparation, in the case of diagnostic hysteroscopy, the device is inserted through the cervix into the uterine cavity. In case of therapeutic intervention, dilation of the cervix is also necessary.
With the help of the camera on the hysteroscope, the inner surface of the uterus, the lumen of the fallopian tubes become visible, and possible lesions can be detected (polyps, myomas, adhesions, developmental disorders, morphological changes, etc.)
What are the risks of the intervention?
- Hypersensitivity reactions to substances used for disinfection or anaesthesia may occur and should be treated with professional care.
- In rare cases, the uterine wall may be damaged during surgery, which may lead to further surgery (laparoscopy).
- In case of lesser-pelvic (uterus, fallopian tubes, ovaries) inflammatory disease, we use a broad-spectrum antibiotic and anti-inflammatory treatment.
