Lumbar spine stenosis surgery
As we age, and due to increased physical exertion, spinal wear (also known as degenerative processes) leads to the damage of the connection between the two vertebrae involved, and the formulas that make up the walls of the spinal canal are deformed. Deformity of the joints, thickening of the ligaments between the vertebral arcs (ligamentum flavum), protrusion of the disc wall causes the stenosis of the spinal canal that runs through the spinal column, which is made up of vertebrae and discs, leading to constriction of nerve elements (nerve roots in the lumbar region) passing through the canal, thus dysfunction.
A classic symptom is that the patient can stand or walk only for a short time because of severe pain and/or numbness in one or both lower limbs. These complaints can be accompanied by lower back pain. Otherwise and in general, the compression of the nerve root in its supply area can cause sensory disturbances, numbness, pain, in more severe cases, the strength of the muscles it supplies may decrease, even increasing to paralysis. Weakening of the sphincter of the bladder or rectum can lead to urinary and defecation disorders, and impotence can occur in men.
When is lumbar spine stenosis surgery needed?
The process usually develops slowly and progresses slowly, in terms of the development of symptoms as well. It is sometimes associated with vertebral slippage, which increases the narrowing of the spinal canal. In many cases, the already formed narrowing can also be aggravated by the herniation of the disc, which, in addition to other narrowing factors, can suddenly increase the number of complaints.
Although the spinal canal can be narrowed for other reasons (tumour, inflammation, bleeding, deformity due to fracture), in the classical sense, narrowing of the spinal canal is understood as a disease that develops on a worn surface.
If the existing symptoms do not improve despite conservative treatments, or if the patient’s condition continues to deteriorate, surgery to dilate the lumbar spinal canal may be necessary.
How is lumbar spine stenosis surgery performed?
Surgical treatment of the disease:
Removal of thickened yellow ligaments (ligamentum flavum), which cause the root canal to stuck, from a posterior, mini-excavation (approximately 3-6 cm) using a microscope, removal of bony elements, and if necessary, disc herniation causing the stenosis of the spinal canal; i.e. increasing the diameter of the spinal canal — called micro decompression.
Surgical procedure:
From a small skin incision, along the middle, rearward-facing, thorny protrusions of the vertebrae, we reach the vertebral arch by splitting the fascia and separating it. Bone release is performed from the vertebral arch at the height of the stenosis by drilling through the opposite side of the opening or under the thorny protrusion, i.e., dilation is performed on the posterior wall of the spinal canal. The thickened yellow ligaments adhering between the arches and under the drilled arch part are then removed on both sides. As a result, the spinal canal is opened and dilated. If necessary, the two sides of the spinal canal are also dilated with drilling device and pliers to remove the deformed joint parts causing the stenosis. If a disc herniation or disc pre-arching significantly narrows the canal, they will also be removed. A suction tube (drain) is left temporarily in the surgical area, and the injury is closed above it.
What to do after lumbar spine stenosis surgery?
In a complication-free case, the patient gets up and walks the day after surgery. From the day after the operation – according to protocol – regular exercises begin. In problem-free case, patients are discharged 1-2 days after the procedure. If an early complication does not develop, the sutures are usually removed after about 1 week, until which it is not advisable to expose the wound to water. The wound can be soaked, you can bathe and swim when the suture line is no longer covered, the wound is completely healed, i.e. the scar is visible (about 4 weeks after the operation).
From the day of surgery until full mobility is achieved, injection therapy (thrombosis prophylaxis) is required to prevent thrombosis, which patients are taught to administer.
After the operation, we recommend that you spare, rest your spine, and that you do a step-by-step physiotherapy, during which it is suggested to avoid persistent sitting (lasting more than 10-15 minutes). Anyone who has experienced severe muscle weakness as a result of damage to a constricted nerve root may also need selective stimulus current therapy aimed at stimulating the weakened muscle. Generally, after 6 weeks, patients return to their sedentary job. Returning to a physical job may happen later (a difficult physical job may require up to 3 months of recovery). In rare cases, recovery may be even slower and rehabilitation may be required for marked initial symptoms and symptoms that persist after surgery.
The final state can be evaluated approx. 1 year after the intervention.
What are the benefits of lumbar spine stenosis surgery?
When the nerve formula(s) is (are) released, it is possible to improve the function, i.e. to reduce the pain radiating to the waist and lower limbs, to reduce the sensory disturbance, and to improve the muscle strength. Lumbar spine stenosis surgery does not guarantee improvement, or becoming completely asymptomatic either, it only provides a chance. Surgery gives an opportunity to avoid possible subsequent paralysis.
What are the risks of the intervention?
Intraoperative complications:
- The chance of damage to the nerve root, cauda fibre, which is stuck next to the space narrowing, is approx. 1.3-2.6% depending on the literature (does not necessarily cause symptoms or permanent damage), consequently a decrease in the function of the nerve element (increase in case of pre-existing damage), which may be a decrease in muscle strength, paralysis in severe cases, sensory disturbance, incoordination, urinary and defecation disorders, impotence in men. Of this, the chance of stool and urinary incontinence is approx. 0.5%.
- Injury to the dura mater (about 11%) in the spinal cord, which contains the cerebrospinal fluid and nerve fibres, as well as radicals, with consequent cerebrospinal leak, which can cause wound healing disorders, may require further surgery.
- Significant blood loss, injury to the large blood vessels running in the front of the spine, which may require a blood transfusion and another surgery (0.05%) if the disc was also affected by the surgery.
Postoperative complications:
- Haematoma in the surgical area, which may lead to repeated narrowing of the nerve elements, might result in another surgery (approximately 0.5%).
- Wound healing disorder, wound infection that may require repeated or multiple surgeries, even with spinal stiffening, as well as antibiotic treatment (approximately 1-3%).
- Chronic low back pain (approximately 7-37%).
Am I suitable for lumbar spine stenosis surgery?
In each case, your doctor will decide, based on preliminary tests, what the risk of lumbar spine stenosis surgery is for you. An anaesthesiologist is also consulted to determine the risk more accurately. The results of the tests and consultation with the anaesthesiologist are crucial.
What is included in the price of lumbar spine stenosis surgery at Medicover Hospital?
The price of lumbar spine stenosis surgery includes the cost of the surgery as well as the cost of post-surgery hospital stay and follow-up examinations.
The implant to be implanted will be determined by the specialist by performing the surgery during the consultation, depending on the case. The price indicated on the page does not include this fee.
The fee for the preliminary specialist consultation and the pre-operative examinations is not part of the surgical cost, please inquire about the cost of these by contacting our Call Center.
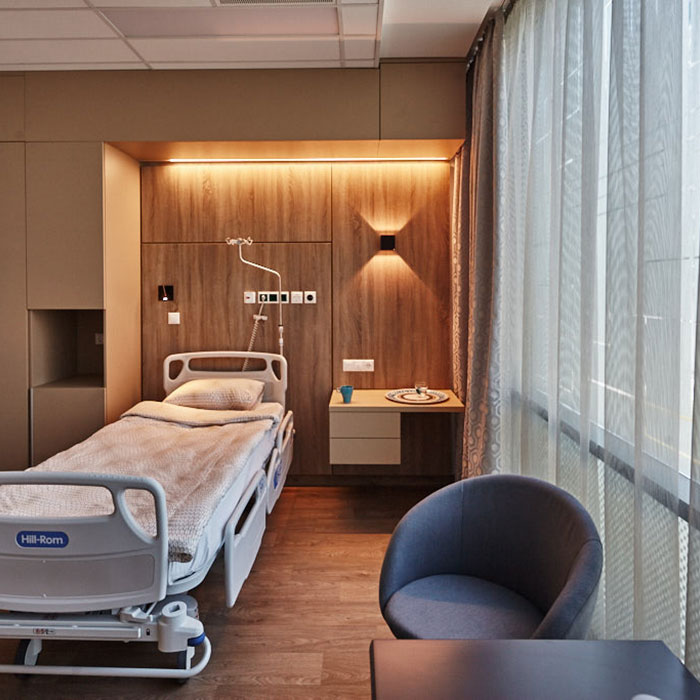
Convenience services
We accommodate our clients in a modern, pleasant, air-conditioned single room. Each room has a private bathroom, fridge and TV, as well as free WIFI access. We also provide our clients with individual nurse supervision, who will help your continuous recovery during your stay.

