Rectal fistula surgery
The purpose of the rectal fistula surgery is to remove a fistula close to the anus. The nature of the surgery depends on the location of the rectal fistula. If it runs superficially under the skin and does not touch the sphincter, a relatively simple surgical procedure is performed, during which the skin is opened under anaesthesia and the inside of the fistula is cleaned. The passage is then left open and allowed to heal from the bottom, similar to a wound.
However, if the rectal fistula is located higher in the rectum and passes through the rectal sphincter, it requires more complicated surgery. It is very important that the rectal sphincter is not damaged during surgery. In this case, the inner opening of the passage is blocked, and as a result – in the absence of supply – the fistula heals on its own.
What is a fistula?
Simply put, a fistula is a pathological change in which a connection is made between organs or body cavities in the body (internal fistula) through which a liquid or solid substance passes unnaturally, or a pathological connection with the outside world is established. These abnormal connections can be congenital, or as a result of an accident, infection, or surgery.
How is the last section of the colon, the rectum, made up?
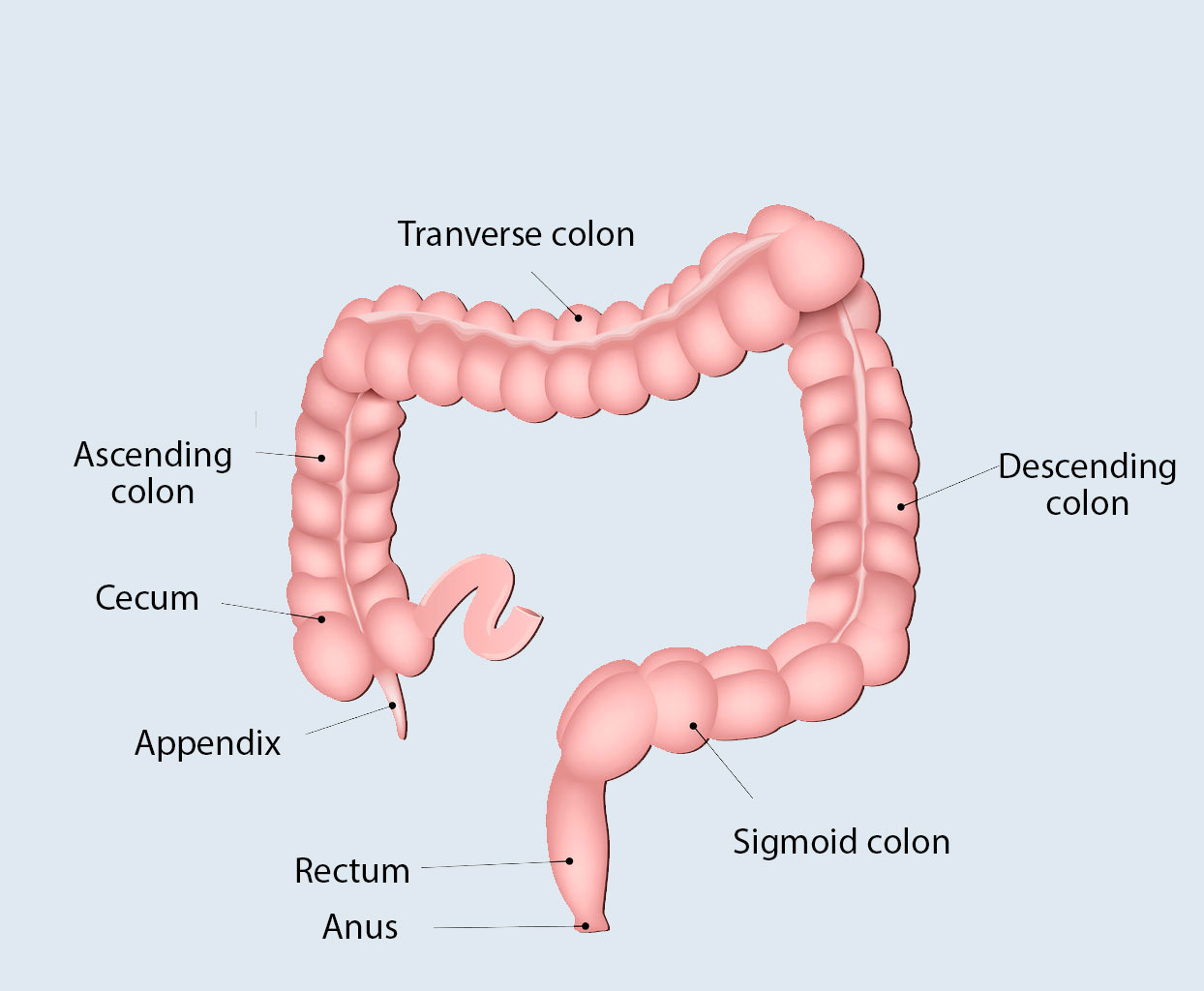
The colon is located in the abdominal cavity, framing the small intestine. It can be divided into several sections: the input part is the cecum, followed by the ascending colon, then the transverse colon, the descending colon, and the sigmoid colon.
The last section of the colon is the rectum, which is located in the pelvis. Of the two curves, the greater lies in the concavity of the sacrum, and the shorter, of opposite curvature, passes through the perineum, fused with its muscles.
The opening of the outlet of the rectal sacrum is the anus. It is operated by two sphincters, the internal, non-voluntary and the external voluntary sphincter. These ensure voluntary stool retention as well as defecation.
The proctologist is a specialist in the lesions and diseases that develop at this stage of the colon.
What causes the rectal fistula to form?
The rectal fistula may be the result of some previous inflammation or abscess, but may result from a perforation caused by a foreign body or Crohn’s disease. It can also lead to the formation of glands in the muscle layers of the intestinal wall that become inflamed. The pus that accumulates as a result of inflammation tends to leave in the tissues around the rectum, creating passages for itself in the process. When it breaks to the surface, it usually appears in the form of an abscess, which is a painful lump near the anus. Rectal abscess is usually associated with fever and requires immediate surgery.
What are the symptoms of rectal fistulas?
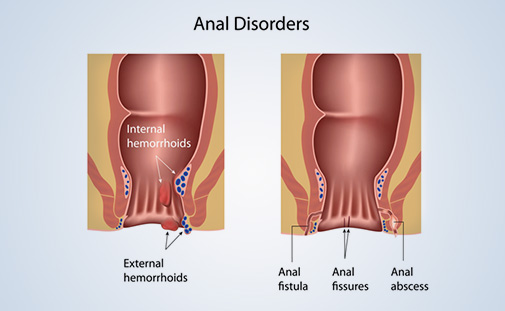
The most common complaint is temporary purulent, bloody discharge but it can occur with shorter or longer interruptions, and temporary straining pain. The consistency and quality of the stool are often related to the intensity of the complaints. If they persist, they maintain chronic inflammation in the surrounding soft tissues, sometimes causing abscesses. This can even impair the function of the rectal muscle.
How can the rectal fistula be diagnosed?
The first and most important part of making a diagnosis is a physical examination, visiting the outer opening of the fistula. During the examination of the passage, the path and course of the fistula and the location of the inner opening can be determined. If it is located high and cannot be reached by a finger, from the rectum, it can be easily determined by contrast-enhanced imaging or X-ray, as this also determines the treatment procedure. If co-morbidity is suspected, colonoscopy may be warranted.
Treatment of rectal fistulas
Chronic fistulas that have been present for several months are expected to be resolved from surgery (rectal surgery). Surgeries of lower, superficial fistulas can be performed under local anaesthesia as part of surgical outpatient care. The wall of the fistula is excavated, excised and, if necessary, rubber threaded. These surgeries do not affect the rectal muscle, so there should be no stool continence disturbance.
Lesions that are higher require a stay in our private hospital, as they require more serious surgery due to the sphincter, and we perform the surgery under general anaesthesia or anaesthesia near the spine. These surgeries involve a stay of 1-3 days, depending on the type of anaesthesia and the type of surgery performed.
Absorbable sutures are inserted during rectal fistula surgery. In the first few days, it is important to provide looser stools that are easier to empty than usual. Because of this, it is necessary to consume plenty of fluids and consume less solid food. It is also advisable to avoid constipation later (fluid, more plant fibre, probiotic treatment). After the pain has dissolved, the movement is not limited. Non-steroidal analgesics may be used to relieve initial pain.
How do I prepare for surgery?
It is extremely important that you are aware of any restrictions prescribed by your doctor, such as not being able to eat solid food the day before the surgery. Make a list of all the medications, vitamins, and supplements you are taking.
Please keep us informed of key medical information, including other illnesses and important personal information such as recent changes in your life or the effects of stress.
All of our patients are asked to complete a detailed medical history form, which is necessary for our surgeons and physicians to decide if you are suitable for surgery.
What can I expect after the surgery?
Since fistulas are very diverse, so is the healing period, its nature is also diverse. Superficial ones heal well, but the healing time in this case can also be measured in months. Higher, branched, or neglected fistulas are much more difficult to treat, in which case they are treated with combined surgeries. For this reason, it is important that you see a doctor as soon as possible if you notice any symptoms.

