Bladder tumour removal
What is a bladder tumour?
During bladder removal surgery, the lesion in the lumen of the bladder is removed. The danger of a malignant bladder tumour lies in the fact that if it is discovered late, it also enters the deeper layers of the bladder wall and forms distant metastases.

How does a bladder tumour develop?
A bladder tumour can be linked to HPV infection, hereditary factors, chemicals (e.g. tar, aniline). It is important to know that it takes a long time for symptoms to appear, and a bladder tumour can go unrecognized for years.
What are the symptoms of bladder tumour?
Painless discharge of bloody urine that is clearly visible to the naked eye, which stops after its initial occurrence and may only recur after weeks or months.
How is a bladder tumour recognized?
A simple abdominal ultrasound can detect in a significant number of cases if the patient is participating in the examination with a full bladder.
In case of suspicion, cystoscopy is performed as part of the urological examination to clarify the presence of the tumour.
How to treat a bladder tumour?
In the case of a proven bladder tumour, it is not possible to apply conservative treatment, only surgery provides a solution to the problem. During the operation, the bladder is examined and the visible lesion is excised and removed to the intact bladder wall. The removed lesion is then sent for histological examination. Having the histological result, we can determine the need for further treatment. You will probably need additional treatments after the surgery, you can discuss these with your doctor.
When is surgery warranted?
In case of a detected tumour, surgery should be performed in each case.
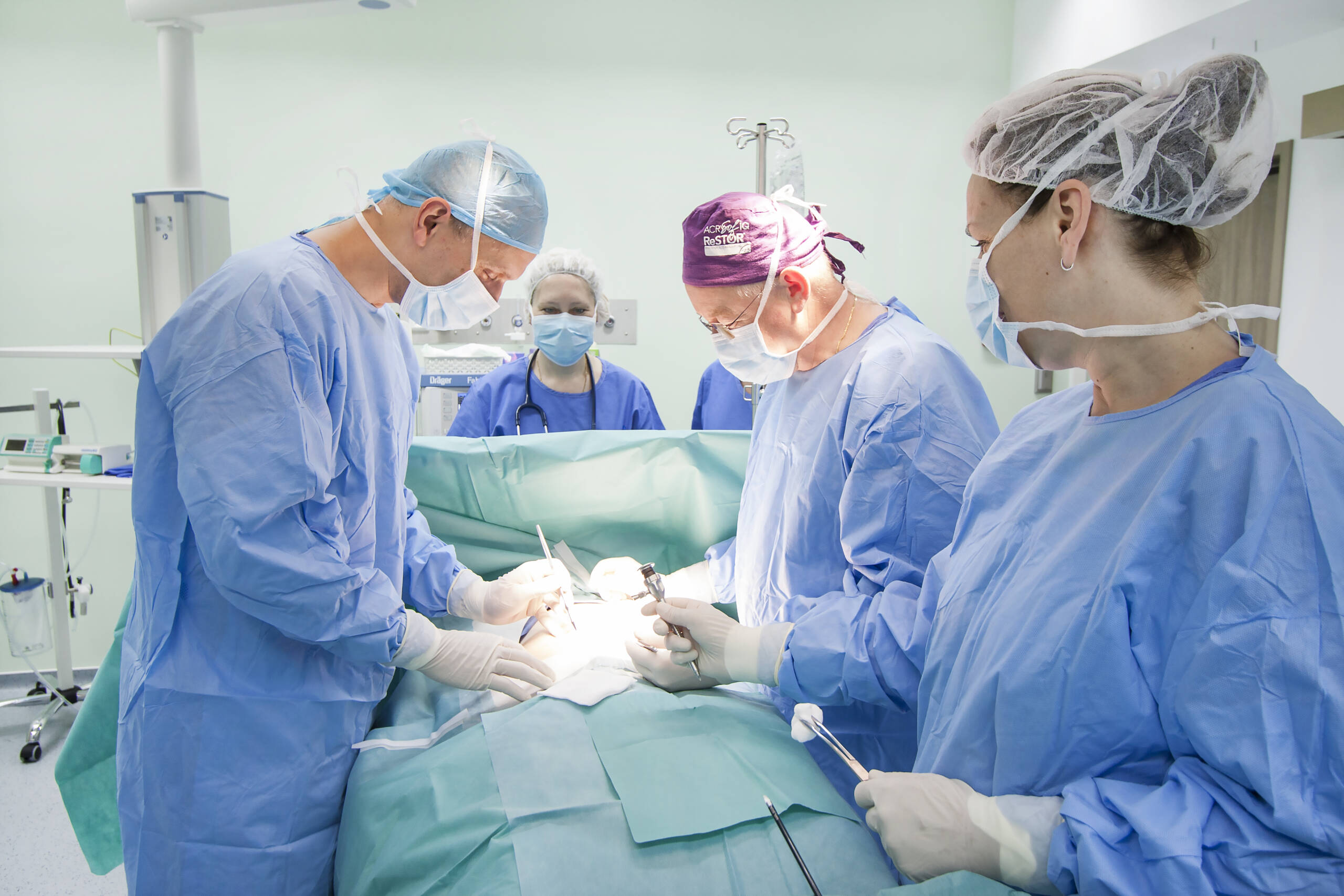
What happens during the bladder tumour removal through the urethra surgery?
After using the anaesthetic method decided by the patient and the anaesthesiologist, an operative endoscope (resectoscope) is inserted into the bladder through the urethra. The bladder is inspected and the visible lesion is excised to the intact bladder wall, removed, and a catheter is inserted into the bladder after careful haemostasis.
However, in some cases, when a small lesion is resected, the catheter is not inserted into the bladder. The removed lesion is then sent for histological examination.
What are the risks of the surgery?
According to the current stance of medicine, no doctor can guarantee the absolute safety of a surgical procedure and the complete success of the surgery. General risks of medical intervention, such as infections, post-bleeding, etc. may occur. After surgery, the previously removed lesion can recur, appear in other parts of the bladder, or narrow the urethra and, in the most severe case, puncture the bladder wall, necessitating immediate surgery. The chances of developing complications are greatly influenced by what previous bladder surgeries have taken place.
Other comorbidities, such as cancer, high blood pressure, obesity, diabetes, haemophilia, and hematopoietic diseases, can greatly contribute to the development of surgical complications. The development of complications is greatly influenced by your age. In general, however, the frequency of complications is negligible relative to the number of surgeries performed.
What to expect after surgery?
After the procedure, there may be mild pain around the bladder. The bladder catheter is removed the day after surgery or within 1 week at the latest. Medication should be used as directed by a doctor to prevent infections and reduce pain. Leaving the hospital is possible at the earliest on the day after surgery. Your doctor will inform you comprehensively about the further possibilities and course of the treatment.
What are the consequences of an untreated bladder tumour?
Failure to intervene may result in the possibility of tumour progression and associated deterioration.
What does the cost of ureteral bladder tumour removal surgery include at Medicover Hospital?
The cost of surgery to remove a transurethral bladder tumour includes the cost of the surgery, as well as the cost of post-surgery hospital stay and follow-up examination.
The price of the preliminary specialist consultation and the pre-operative examinations is not part of the surgical cost, please inquire about the cost of these by contacting our Call Center.
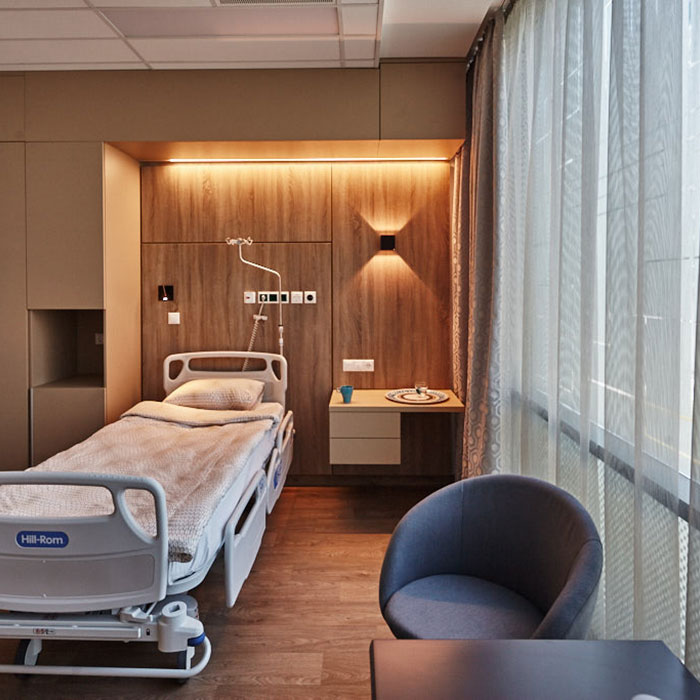
Convenience services
We accommodate our clients in a modern, pleasant, air-conditioned single room. Each room has a private bathroom, fridge and TV, and free WIFI access. For our clients, we provide individual nurse supervision, who will help your continuous recovery during your stay.

