Proctology
What is proctology?
Proctology is a medical specialty within general surgery, which deals with the examination, diagnosis, and treatment of the diseases of the rectum.
Rectal diseases include, for example, external and internal haemorrhoids – affecting about 40% of adults over the age of 50 – and long-term asymptomatic colorectal cancer, one of the most common fatal diseases among cancers.
In addition, proctology deals with various inflammatory processes in the rectum, benign and malignant lesions and the examination and treatment of anal fissure.

With what symptoms is it recommended to see a proctologist?
Contact a proctologist if you have the following complaints:
- Bloody mucus secretion
- Itching around the rectum
- Wart-like lesions around the anus
- Rectal pain
- Bloody stools
- Feeling of a foreign body in the rectum
What diseases does the proctologist treat?
Haemorrhoids
Haemorrhoids are a dilation of blood vessels that are located under the skin surrounding the anus, or on the inner wall of the rectum. Internal haemorrhoids are painless in most cases but may indicate the presence of bleeding during defecation. The main symptoms of external haemorrhoids are pain, itching and, in certain cases, bleeding during defecation. Haemorrhoids can be caused by straining during defecation, malnutrition (insufficient fluid intake, excessive alcohol and spicy food consumption), obesity, connective tissue weakness, and hormonal changes during pregnancy.
At our clinics, we perform anoscopic haemorrhoid ringing as part of outpatient care. In our hospital, we perform haemorrhoid surgery in two ways: using a traditional procedure (removing and covering the supplying arteries by removing the wide hemorrhoidal pads) and using the Longo technique.

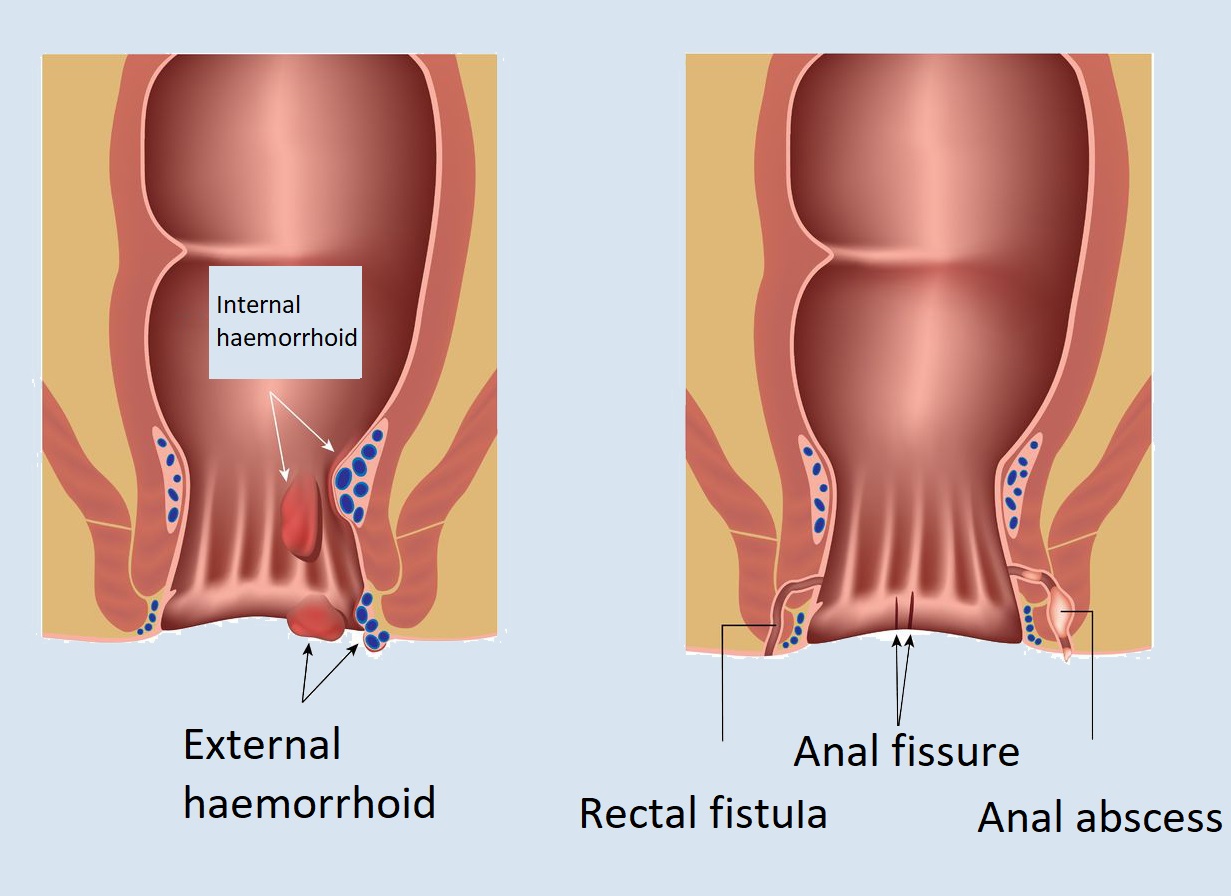
Anal fissure
Anal fissure is the rupture of the rectal mucosa, which in more severe cases can develop into a mucosal ulcer. The most common symptom is pain, which in some cases is mild, or burning, but in other cases it can be very intensely stinging and convulsive. Additional symptoms may include bleeding. It can develop as a result of inflammation of the rectum, colds, diarrhoea, constipation, or birth trauma. At an early stage, the rupture may disappear without a trace with medication (suppository). If necessary, in our hospital, the lesion is excised together with the skin tag, and then, the mucosa is reconstructed with absorbable sutures if needed.
Rectal fistula
The fistula is an abnormal connection of natural body cavities or hollow organs and their abnormal discharge to the body surface. The rectal fistula may be the result of some previous inflammation or abscess, but may develop from a perforation caused by a foreign body or Crohn’s disease.
The most common symptoms are straining pain and occasional (with more or less interruptions) purulent, bloody discharge. If it develops into an abscess, it can impair the function of the rectal muscle.
The non-melded abscesses can be forced to retract with occlusive dressing and a sitting bath can in some cases. When a purulent process develops, extensive surgical exploration is performed. Detailed information on surgical anaesthesia is provided by the anaesthesiologist. The wound is treated open, and regular dressing changes are performed after excision.
Antibiotic protection is provided according to the degree of inflammation. The duration of the abscess excavation is within half an hour. The only way to treat persistent rectal fistulas is to explore the passage, excise the wall, and the open treatment of the wound.
Rectal polyp
A rectal polyp is an outgrowth formed in the rectum, which is the last section of the colon. It affects more than a third of the population. It is more common in people over 50 years of age. It can be a benign or a malignant lesion. There are several sizes and shapes of rectal polyps. While small rectal polyps usually do not cause complaints, larger ones may show symptoms such as bloody, mucous stools, or diarrhoea or abdominal pain. In more severe cases, they can cause not only constipation but also intestinal obstruction. The risk of developing rectal polyps is greatly increased by poor nutrition (low-fibre diet), smoking, excessive alcohol consumption, and genetic predisposition. Certain types of polyps penetrate the intestinal wall a few years after their formation and then develop into a malignancy (carcinoma). The type of a given polyp can be determined by histological examination. Removal of the rectal polyps usually happens at the same time as the bowel endoscopy, when it is discovered.
During the removal of the rectal polyp, the surgeon removes the polyp itself after dilating the anus and undercutting the polyp.
The course of the proctological examination
As a first step in a proctology practice, the specialist asks the patient about the symptoms: what exactly they have experienced, how long the complaints have been persisting, how often they occur. The proctologist then asks questions about the patient’s eating and lifestyle habits and what illnesses have occurred in the family.
This is followed by an external physical examination and, if necessary, an instrumental examination: anoscopy or rectoscopy.
Anoscopy is a device examination to examine the anus as well as the lower 3-4 cm section of the rectum. After the insertion of the anoscope, the proctologist examines the condition of the epithelium and mucous membranes covering the rectum, as well as possible diseases of the anus: internal haemorrhoids, rupture of the rectum, inflammation of the rectal mucosa and tumours of the last section. The advantage of the examination is that the internal haemorrhoid causing the complaint can be treated simultaneously through the thin tube with special devices, but it is also possible to take a tissue sample with a small pliers. The examination is usually painless, however, if it is performed to look for haemorrhoids or rupture of the rectum, burning, stabbing pain may occur during insertion of the device.
For the treatment of internal haemorrhoids, we also perform anoscopic haemorrhage ringing in our clinics in the framework of outpatient care, during which a rubber ring clamping is placed on the internal haemorrhoids with special devices developed for this purpose. With one treatment, only 1-2 rings can be put on, so recovery is expected after several interventions. Regular, loose stools and the avoidance of excessive physical exertion are recommended after treatments.
Depending on the complaints, the examination is often supplemented by rectoscopy to make an accurate diagnosis. During rectoscopy, the last 10-20 cm section of the colon is examined by a proctologist by inserting a special instrument. The test is performed for diagnostic purposes, with the help of which benign (polyps) and malignant lesions of the rectum, as well as inflammation, ulcers and stenoses can be detected in time. Sampling (biopsy) and removal of polyps are also possible during rectoscopy. The test only takes 1-2 minutes, can be uncomfortable, but does not cause pain.
If the above-mentioned examinations are not sufficient, either colonoscopy, X-ray or biopsies may be required, which are carried out during a separate consultation
Proctological procedures
- Anoscopic examination for internal haemorrhoids, rectal fissure or to diagnose inflammation of the rectum
- Treatment of haemorrhagic problems (external and internal haemorrhoids)
- Haemorrhoid ringing
- Rectoscopic examination to detect benign and malignant rectal lesions as well as inflammation, ulcers and stenoses
- Histological sampling (biopsy)
- Colonoscopy
- Removal of rectal polyps (smaller, benign tumour)
- Rectoscopy
Proctological surgical procedures available at Medicover Private Hospital
- Rectal polyp surgery, rectal polyp removal
- Haemorrhoid surgery with traditional and Longo procedure
- Surgical treatment of rectal fissure, rectal fistulas, small rectal abscesses
How to prepare for the proctological examination?
Our proctologists can send our clients for laboratory tests to make an accurate diagnosis and recommend the imaging diagnostic procedures available at the Medicover Advanced Diagnostic Center: X-ray, ultrasound, CT and MRI examinations.
Proctology is also available at our clinics in Budapest as part of outpatient care. Contact our Call Center for the prices of proctological examinations.

