Laboratory testing of female sex hormones
In the female sex hormones laboratory package, we examine cycle-dependent female sex hormones in case of bleeding disorders and infertility problems. Cycle-dependent hormone levels are monitored by two blood draws on day 3 (AMH, FSH, LH, testosterone, prolactin, oestradiol) and day 21 (progesterone) of the cycle.
For women taking contraceptives, the result cannot be evaluated, so it is recommended that a laboratory test be performed after leaving the contraceptive.
The first blood draw takes place on day 3 of the menstrual cycle (AMH, FSH, LH, testosterone, prolactin, oestradiol). The first half of the cycle is the follicular phase and the period after ovulation is the luteal phase. At the first blood draw (H1), we examine a complete line of hormones, when problems arising from the functioning of glands and organs that produce hormones can be revealed, so we get a general picture of hormone homeostasis and organ function, that is, whether the uterus is able to receive a possibly fertilized egg. The second blood draw of cycle-dependent hormones takes place on day 21 (progesterone).
In the second half of the cycle, a repeated female hormone test (H2) on day 21 seeks to clarify whether hormonal processes are developing properly, whether the fertilized egg could be implanted in the uterus, whether there is corpus luteum insufficiency, or other problems.
AMH (anti-Müllerian hormone)
Its examination provides an opportunity to assess the reserves of the ovaries. Hormone levels gradually decrease during the female fertility phase, which is associated with a decrease in the number of eggs/follicles with age. Estimation of ovarian reserve can predict the success of ovarian stimulation as well as the time remaining until menopause.
Conditions with elevated AMH levels may include polycystic ovary syndrome (PCOS) and ovarian granulosa-cell tumours.
FSH
FSH (follicle-stimulating hormone, follicular maturation hormone) is a sex hormone produced in the anterior lobe of the pituitary gland. Although FSH and LH are required for normal sexual function in both men and women, the process of excretion in the body is very different for the two sexes.
FSH initiates the growth and development of ovarian follicles. During ovulation, the follicle ruptures, the egg is released and the corpus luteum forms. In menopause, decreased ovarian function results in a decrease in oestradiol secretion, resulting in a significant increase in circulating FSH levels.
When may the test be needed?
Diagnosing menstrual disorders, infertility, menopause, pituitary gland and diseases associated with ovarian disorders.
When a woman reaches menopause and her ovaries stop functioning, FSH levels rise.

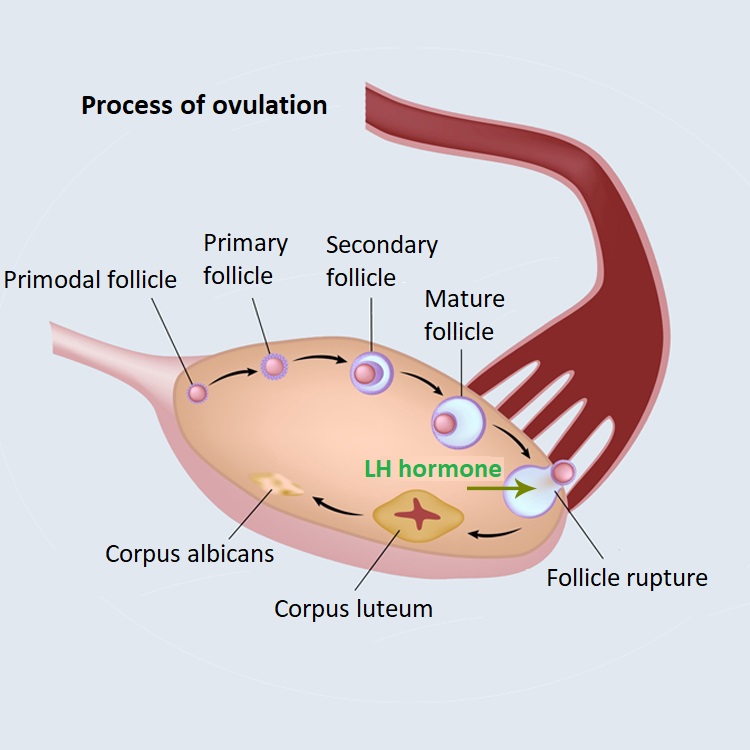
LH (luteinizing hormone, corpus luteum stimulating hormone)
LH is a sex hormone that is produced in the anterior lobe of the pituitary gland. LH triggers ovulation (follicular rupture). It further matures the follicle prepared by FSH; when LH levels increase, ovulation occurs. LH also stimulates the production of steroid hormones (oestrogen and progesterone) in the ovaries.
During menopause, when the ovaries stop working, LH levels remain elevated.
For infertile women with reduced fertility and for infertile women treated with gonadotropins, its determination may provide information about the onset of ovulation.
When may the test be needed?
Diagnosing menstrual disorders, infertility, menopause, and diseases associated with ovarian and pituitary gland disorders. When a woman reaches menopause and her ovaries stop functioning, LH levels rise.
Other causes of missing follicular rupture may include: polycystic ovary syndrome (PCOS), adrenal gland disease, thyroid disease, ovarian tumour.
Prolactin
Prolactin is a hormone produced in the anterior lobe of the pituitary gland. There is a slightly higher value in women than in men. During pregnancy, prolactin levels rise directly to ten to twenty times the normal value and then fall back to normal levels in mothers who do not breastfeed within three weeks of delivery. In case of breastfeeding, the decrease occurs gradually to normal levels. It stimulates milk secretion and inhibits the production of hormones responsible for initiating the female sexual cycle after childbirth, i.e. follicular maturation.
Causes of high prolactin levels can be:
- stress, sleep, pregnancy, post partum, physical work, breastfeeding
- drugs (e.g. oestrogens, sedatives)
- decreased thyroid function,
- renal and hepatic insufficiency,
- polycystic ovary syndrome
Testosterone
Testosterone is secreted in small amounts by the adrenal glands and ovaries in the female body. It affects skeletal muscle development and body fat distribution, and reduces the excretion of nitrogen, sodium, potassium, chlorine, phosphate and water in the urine. Testosterone is converted to oestradiol, the main female sex hormone.

Oestradiol
It is a member of the oestrogen family (estrone, oestradiol, estriol). In women, it is mainly produced in the ovaries and placenta. Adequate levels are needed for egg maturation, conception and pregnancy, as well as maintaining healthy bone mass. Additionally, it is involved in the regulation of cholesterol levels and the development and maintenance of secondary sexual characteristics. Oestradiol levels increase during pregnancy as the placenta also begins to produce it. During menopause, oestradiol production becomes irregular and occasionally paused.

Progesterone
It plays an important role in the formation and maintenance of pregnancy but is also partly responsible for regulating the female menstrual cycle. It is produced mainly in the placenta and ovaries, but a small proportion is also produced by the adrenal cortex in both sexes. Circulating progesterone levels are typically low in the first phase of the cycle and then increase steadily in the second phase of the cycle, reaching their peak 5–10 days after the mid-peak LH peak (days 21–22 on a 28-day average cycle). If pregnancy does not occur, it drops sharply to the level in the first half of the cycle (almost zero).
Cycle-dependent hormone levels are monitored by two blood samples, and the laboratory test should be performed on days 3 and 21 of the cycle.
How do I prepare for the test?
Having an empty stomach is not required for female sex laboratory test.
When is the result expected?
After the 5th working day following the test.

