Chondromalacia patellae (cartilage softening) surgery
What is chondropathy?
Cartilage softening is a degenerative (worn out or arthrosis) lesion that affects the structure and function of the whole knee joint. First, the cartilage structure that covers the joint surfaces changes: the former smooth surface becomes fibrous, cracked, “softens,” and then deeper fissures form on it, and the cartilage cover peels off in places. At the end of the process, completely cartilage-free parts are formed, which mainly causes pain and a loss of function in the joint.
However, arthrosis not only affects the cartilage surfaces, but also affects the structure of the bone below the cartilage: in some cases thickening, in some cases small bone cavities, so-called degenerative cysts are formed – the cavity of the latter is connected to the joint, and the synovia squeezed into them during movements can cause severe pain. The arthritic condition causes continuous inflammation of the synovial membrane and can cause shrinkage, thickening, and even partial calcification of the sheath surrounding the joint. On non-load-bearing surfaces, i.e. on the edges of the joint, characteristic bone deposits form, which deform the articulating bone ends and can stretch the joint capsule.
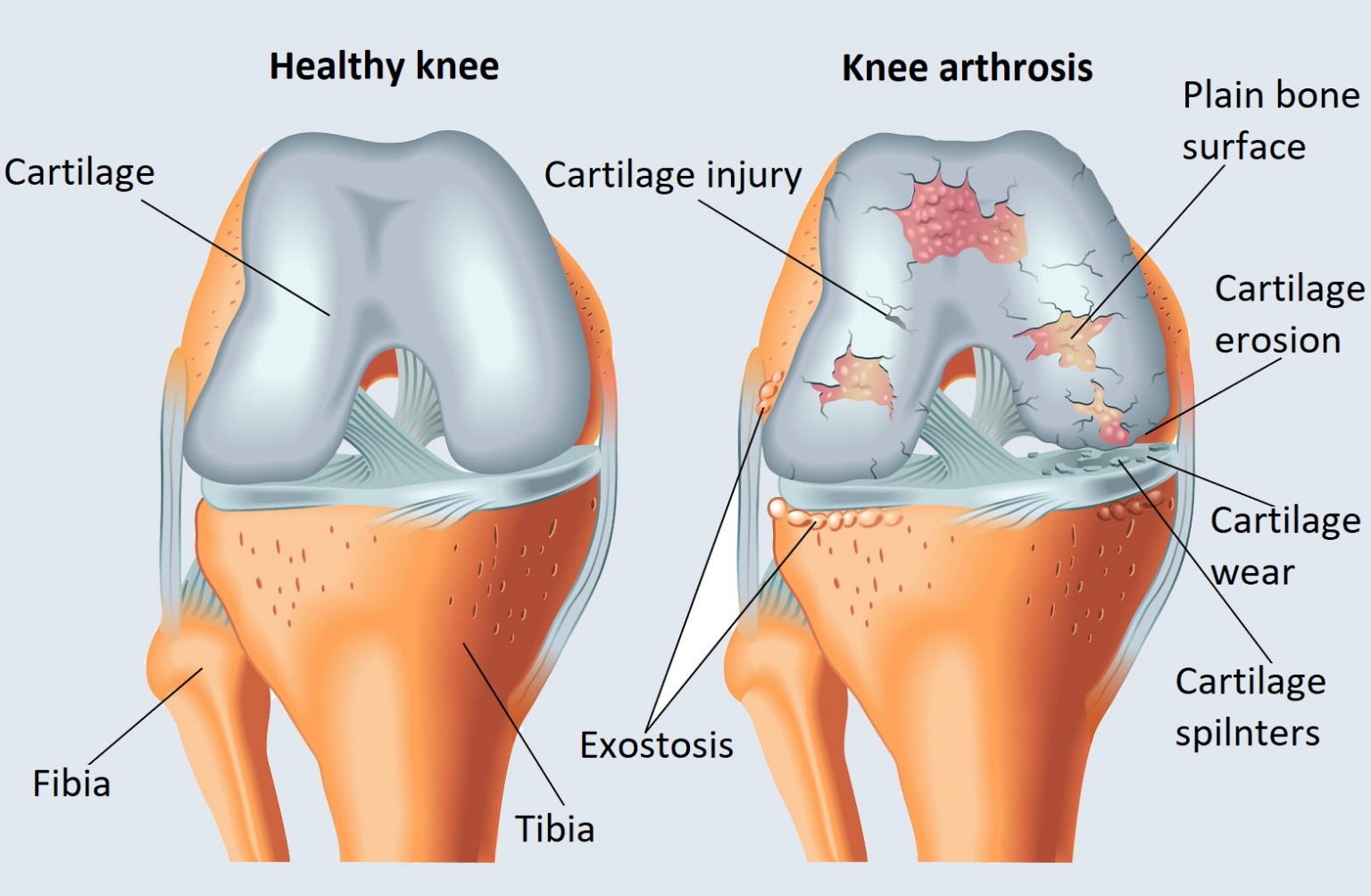
How does cartilage softening develop?
Arthrosis appears in all joints to some extent with age, but the occurrence frequency and severity are very different: mostly the small joints of the hands, hips, knees, and spine are affected. As this shows, abrasive lesions are mainly associated with age and joint wear but there are factors that can accelerate these processes: for example, a change in joint structure due to a previous injury, or some disease affecting the joints. Like so many other musculoskeletal disorders, it is true of arthrosis that genetic factors also play a role in its development.
What are the symptoms of cartilage softening?
Complaints appear more intensely and discreetly, regardless of the size, depth, and location of the lesion:
- pain under load,
- crackling during movement, feeling of jamming,
- joint swelling,
- strain, warming and fatigue.
Symptoms can occur in a variety of ways; hindering straining and exercise, but the asymptomatic period can persist for a long time. Complaints cannot usually be localized to a specific location.
How is cartilage softening diagnosed?
In case of cartilage surface damage, it is important to make an accurate diagnosis, which is done by a knee specialist orthopaedist. The examination includes a physical examination, a stress X-ray examination or an MRI scan. The extent of cartilage surface damage is revealed during arthroscopic surgery most accurately.
What treatment can cure cartilage softening?
In the case of surgical treatment of cartilage damage (cartilage softening), the primary goal is to control the lesion and possibly initiate regeneration processes at the site of the damage. To stop further detachment of the degenerate cartilage parts, the detached, fibrous cartilage must be removed and the surfaces smoothed.
The mechanical role of “shaving” in the process of restoring joint function lies in the fact that the regeneration process begins in the treated areas. The surfaces are tightly covered with a fibrous cartilage cover layer, therefore its wear is slowed down as a coating layer is formed on the surfaces.
If we are faced with greater cartilage surface damage, cartilage surface stimulation follows the cleansing of cartilage surfaces, the so-called microfracture (drilling) is considered to be the safest routine procedure. With proper rehabilitation, the affected area can develop a so-called hyaline cartilage-like fibrous cartilage, which, although histologically and from a load-bearing perspective, does not correspond to the original hyaline cartilage, in many cases an excellent chargeable cartilage surface is formed.
What can I expect after the surgery?
In the first few days after surgery, the joint will recover from the stress of the operation. Rest is required because during arthroscopy, the joint lubricant is “washed out,” and it takes three days for the synovial fluid to regenerate.
After cartilage surgery, complete relief for 6-8 weeks with two crutches is crucial. When this period passes, the operated surface becomes strong enough so that the coating layer would not tear off, and even a small load and stepping on the foot does not compress the cartilage surface.
Only the physiotherapy prescribed by the physiotherapist can be performed with the operated leg, at which time the muscle strengthening and stretching exercises can begin. If the relief does not happen consistently or the physiotherapy starts too early, the process of surface coating is delayed, the surfaces are practically plain, therefore the harmful enzymes can enter the synovial fluid almost unhindered from the bone. Thereby, the wearing process continues, even if an improvement was observed in the short term. To make the regeneration process even more intense in the treated areas, a cartilage-protective injection of hyaluronic acid or polynucleotide can be given into the joint after a few weeks.
